
The Greater Manchester (GM) i-THRIVE Programme team spoke with Dr Jenny Davies, Principal Clinical Psychologist, Humaira Khalid, Assistant Psychologist, and Christine Chester, Child and Adolescent Psychotherapist from Pennine Care NHS Foundation Trust, and Kirsteen O’Keeffe, Specialist Health Visitor, Stockport NHS Foundation Trust.
Download this implementation story.
Background
There is substantial evidence emphasising the importance of the strength of our earliest relationship with our main caregivers (typically a parent) and its impact on our physical, emotional, cognitive and social development. This early relationship is a key factor in determining resilience, wellbeing and the extent to which individuals will prosper in future education and employment, and relationships with partners and children. Research has shown that up to 30% of parents will struggle to recognise and respond accordingly to their baby’s needs, putting the development of secure attachment at increased risk.
Image 1: Documents highlighting the importance of parent infant wellbeing services

The Stockport Integrated Parent Infant Mental Health Care Pathway
The Stockport Integrated Parent Infant Mental Health (PIMH) Care Pathway is informed by the strong evidence base emphasising the importance of supporting child development and family relationships in the early years of a child’s life.
The PIMH care pathway was developed to promote knowledge and skills amongst professionals in understanding parental mental health and parent-infant relationships. The care pathway helps guide all professionals working with parents during pregnancy and early years. In line with NICE guidance (2014) this includes the workforce from health, education the local authority and the voluntary/private sectors. The aim of the PIMH care pathway is to help improve the emotional health and wellbeing of infants and young children and to contribute to improved school readiness.
In spring 2019 the PIMH care pathway was updated by the PIMH task group, which includes the IAPT service, midwifery, Home Start, Social Care, Perinatal CMHT, Parenting services, Adult Mental Health Team and the Parent Infant Service. The care pathway is a live document that will continue to be updated by the PIMH task group as services develop and change.
Image 2: Flow chart to help professionals and parents/carers decide which service might be best placed to meet identified needs
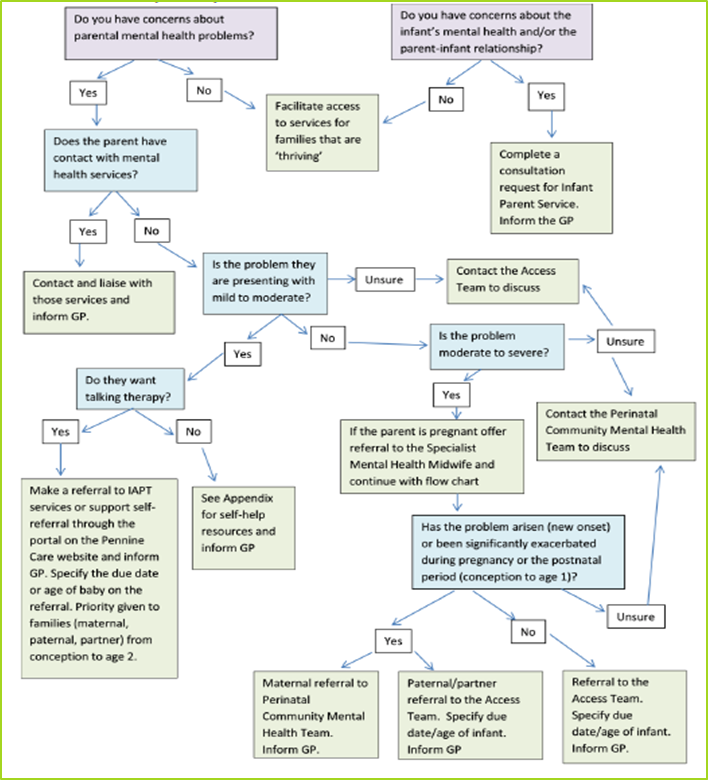
How does the development of the PIMH care pathway align with the THRIVE Framework for system change?
The principles and language of the THRIVE Framework for system change (Wolpert et al., 2019) were utilized in the development of the PIMH care pathway and in the consideration of building services differently. A mix of multi sector agencies mapped out their offer within the care pathway aligned with the THRIVE Framework needs based groupings; enabling Stockport to incorporate whole system working within parent-infant mental health services.
The care pathways and collaborative working between agencies facilitates appropriate services for families, aligns support available in Stockport with the THRIVE Framework needs based groupings, and further facilitates professional knowledge and understanding of their own roles, as well as those of other cross-sector services.
The care pathway enables families to access and make use of the extensive support and intervention offered in Stockport, according to their choices, requirements and needs. The care pathway allows for clear communication between all professionals where there are concerns about parental wellbeing and the parent-infant relationship. The care pathway is an excellent example of shared decision making in practice, with a focus on building individual and community strengths to ensure children, young people and their families are active decision makers in the process of choosing the right approach and support for them.
The Stockport Infant Parent Service
The Stockport Infant Parent Service (IPS) was commissioned jointly by Pennine Care and Stockport NHS Foundation Trusts, as a service dedicated to promoting infant mental health and positive parent-infant relationships from conception to five years of age.
The IPS has a key role in working across parent and infant services, allowing close interagency working between professionals and the parent and child, with a strong emphasis on consultation and training within the service. The IPS team believes that capacity building through workforce training is an integral part of the system, and thus co-deliver a number of multi-professional training events and conferences as well as offering drop-in support for professionals working with families who may benefit from the IPS. The IPS team consists of a Clinical Psychologist as a clinical lead, a Specialist Health Visitor and two Assistant Psychologists all of whom work part-time, as well as a full time Child Psychotherapist.
Referrers have initial conversations with families about the IPS team and discuss if a referral into the team is the right support the family needs. This conversation is a collaborative shared decision making process with families to ensure families are receiving the right support for their current needs. The IPS team reviews referrals into the team in weekly team meetings and allocate cases to team members dependent on skills required. A consultation with the referrer is then booked; following which, the IPS team either work directly with the family or will offer further consultation with the referrer as is appropriate and as has been jointly agreed. Joint visits may be arranged between the referring service and the IPS team member.
Figure 1: Stockport Infant Parent Service offer aligned with the THRIVE Framework
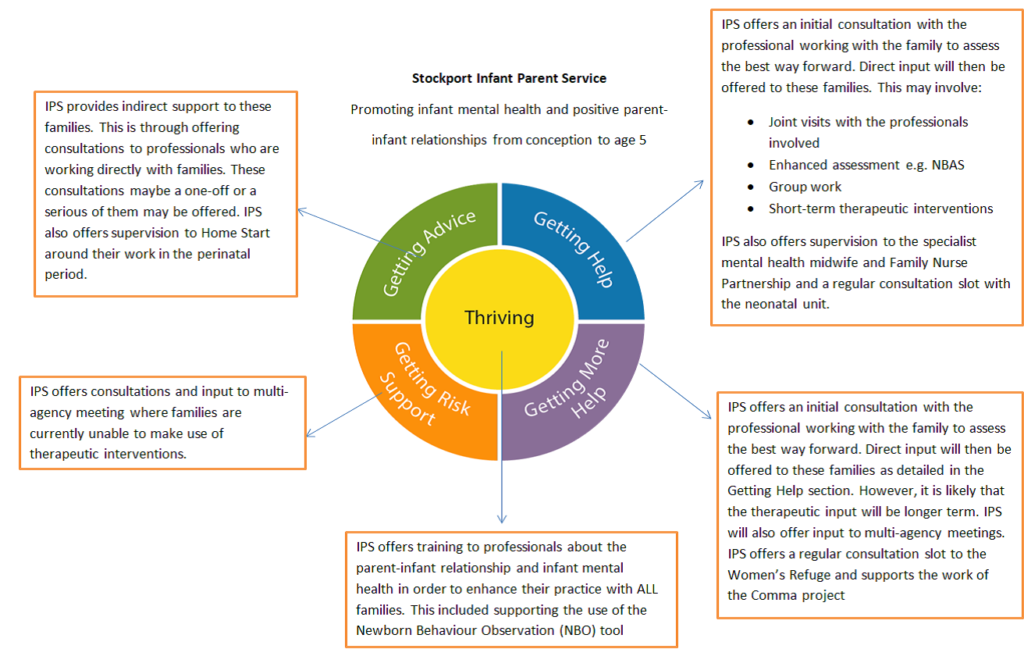
What are some of the challenges faced in developing the care pathway?
Team members in the Infant Parent service are employed by different providers which can make joint-working difficult. However, due to using the same IT record keeping system, wider case discussion can be facilitated due to easy access to information. Moreover, weekly team meetings/weekly allocation meetings also take place to ensure good communication and collaborative practice.
How has the care pathway changed things for staff and service users?
Early intervention from the Infant Parent Service and the use of collaborative methods have shown positive outcomes for the emotional health and wellbeing of the parents and young children seen within the service. The service has received positive feedback regarding the ease of the consultation process, as well as the service’s general availability and offer of helpful information and support.
Comments from professionals:
“Thank you for your input into this family and to child, and for the difference you have made, no more screaming and his development is catching up.”
“Thank you for the work with child, Mum still says what a difference it has made to her understanding and enjoyment of her child.”
“This has been an outstanding piece of work for this Mum and baby; she now feels she knows how to talk to her baby.”
Comments from families:
“Understood mine and my child’s needs. Easy to chat to.”
“Very supportive and easy to talk to which enabled me to work through the issue. Some practical tips to try. Signposts you to other services.”
“Help, make me strong, I feel happy; I feel so proud of myself.”
“[Team member] was lovely. Made me very comfortable and easy to talk to.”
“[Team member] listened very careful about everything we said. We are very happy about [team member] visits and [the] tips we get.”
What is the future of the Parent Infant Mental Health (PIMH) care pathway?
The PIMH pathway will continue to be updated as services develop to enable easy access for professionals and families across Stockport. In implementing the care pathway, the service will continue to co-deliver training and consultations for professionals. The service will continue to evaluate family’s experiences of the service and collect outcome measures to further inform practice.
If you would like further information, please email; snt-tr.infantparentservice@nhs.net.





Edited by the Greater Manchester i-THRIVE Programme Team and National i-THRIVE Programme Team.
Written May 2020.